Authors: Nancy Fliesler
Source: Medical Xpress
Treating children with epilepsy has traditionally been a matter of trial and error, trying different drugs one after the other. In the one-third of patients for whom the drugs do not work and seizures continue, doctors consider brain surgery—if it can be done safely.
Early in her career, Ann Poduri, MD, MPH, who directs the Neurogenetics and Epilepsy Genetics programs at Boston Children's Hospital, wondered: What could be learned from the brain tissue removed during surgery? Could it yield a better genetic understanding of epilepsy?
"If we could know what caused epilepsy for these individuals, maybe we could actually treat them with science on our side," she says.
When Poduri was in medical school in the late 1990s, only three or four epilepsy-related genes were known. Today, through work in her own lab and many others, that's swelled to more than 800.
A genetic diagnosis can mean a change in a child's medications, better planning for the future, and guidance for family members who may share the same genetic variant. Occasionally, it can spark the use or development of new epilepsy medications—with the help of Poduri's zebrafish models—adding to an arsenal that's changed little in more than 20 years.
Poduri's passions also lie in making genetic diagnoses accessible to families routinely, with as little delay as possible. "Early diagnosis means children don't have to keep having MRIs and spinal taps," she says. "With a genetic diagnosis, whether it's good news or bad news, families can have closure and certainty, and important decisions can be made."
Whole-genome sequencing for infant seizures?
A new study published in The Lancet Neurology—the first of its kind—takes a bold step in that direction. Through the International Precision Child Health Partnership (IPCHiP) co-founded by Boston Children's in 2021, researchers at Boston Children's and other centres in Australia, England, and Canada performed rapid whole-genome sequencing of DNA from 100 infants with new-onset epilepsy and, in most cases, their parents.
This approach isn't the norm today clinically. "A typical scenario for a baby with epilepsy is a short clinic or hospital visit that doesn't include discussion of possible genetic causes or how to test for them," Poduri says. "When an infant is on multiple medications, having seizures, and not meeting developmental milestones, there are so many acute issues to be addressed that there's often no time to get to genetics. And most centres don't have genetic counsellors or other professionals who can navigate genetic testing for families."
Whole-genome sequencing is also not the norm in the clinic. Typically used only in a research setting, it is more expensive than whole-exome sequencing, which looks only at the DNA sequences, or genetic material, that code for proteins. But it can solve more cases, identifying mutations in regulatory elements and duplications and deletions in the genome that can also cause disease.
"We wanted to provide evidence that rapid genome sequencing really does have a clinical impact," says Alissa D'Gama, MD, Ph.D., a clinical fellow in Neonatal-Perinatal Medicine who is in Poduri's lab and is first author on the study. "Sometimes it can happen in an intensive care setting, but not a lot of payers will pay for rapid testing in outpatient or other inpatient settings. We hope our work will influence future policy decisions."
Making the case for rapid whole-genome sequencing
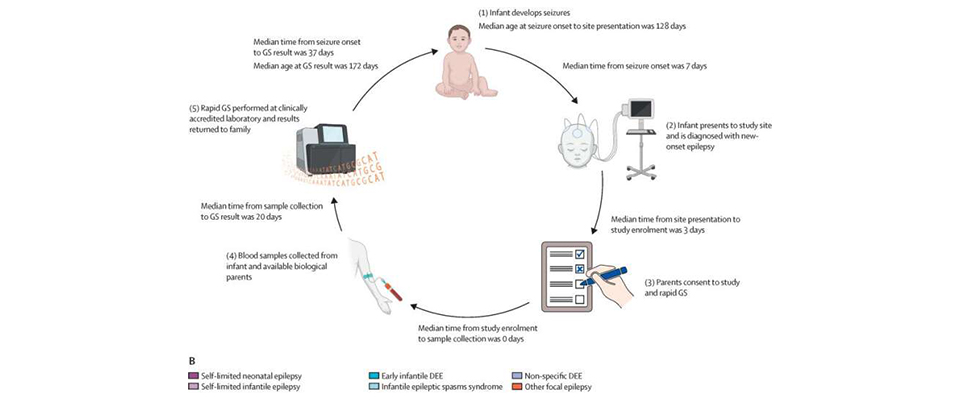
Of the 100 infants in the study, whole-genome sequencing provided diagnostic information for 43, usually within two to three weeks of enrolling in the study. The median time from an infant developing seizures to getting a sequencing result was 37 days.
Diagnostic sequencing results influenced treatment decisions in 24 of the 43 infants (56%), pointed to potential precision therapies for 49%, and provided new prognostic information for 86%. In 28% of cases, the diagnosis had health implications for parents or led to other family members being tested. Overall, sequencing was clinically useful for 55% of the entire cohort, whether families received a diagnosis or not, and whether the prognosis was good or poor.
The study also showed that rapid whole-genome sequencing is feasible in multiple care settings. Diagnostic yields were 30% for infants seen in the outpatient setting, 44% for infants admitted to non-intensive inpatient care, and 71% for infants in intensive care.
"Prior studies of rapid sequencing have primarily enrolled from intensive care settings and haven't focused on a specific disease cohort," notes D'Gama.
From discovery to implementation
Poduri and D'Gama hope their findings will help make whole genome sequencing routine for infants with epilepsy. "The barriers to precise diagnosis and precision treatment are no longer scientific knowledge barriers," Poduri says. "We want to make the so-called 'impractical' practical and accessible for all children with epilepsy."
She and her team are educating clinicians and payers about the value of epilepsy genomics, working through professional epilepsy and neurology societies. They are also looking to partner with neonatal intensive care units (NICUs) in the community and provide genomics services to clinics with underrepresented populations.
"If patients can't get to us, what if we try to get to them? What if we go to other locations and provide translators?" Poduri says. "We have eager young people ready to go out and carry this forward. It takes a whole health system to come together and say, 'Let's make this available to our patients.'"
More information
This article was from Medical Xpress and was legally licensed through the DiveMarketplace by Industry Dive. Please direct all licensing questions to [email protected].

Disclaimer: Novartis Ireland Limited accepts no responsibility for the content, accuracy, interpretation or use of the information contained within this article or its use of linked websites.